Hypothesis
Magnesium 4: 53-59 (1985)
Quantifying the Role of Magnesium in the Interrelationship
between Human Mortality/Morbidity and Water Hardness
J.R. Marier
Biological Sciences Division, National Research Council of
Canada
L.C. Neri
Epidemiology Division, University of Ottawa, Ottawa,
Canada
Key Words. Magnesium - Cardiovascular
system - Ischemia - Blood pressure - ECG Arrhythmias - Drinking
water
Abstract. An attempt has been made to
quantify the effect of waterborne magnesium on human
mortality/morbidity, based on epidemiological and clinical
observations reported in several regions of the modern-day
world. A consistent pattern has emerged, indicative of a global
phenomenon, which illustrates the importance of waterborne
magnesium in protecting against cardiovascular trauma and other
ailments. These findings attest to the inadequate metabolic
magnesium status among modern-day humans, especially those who
reside in ultra-soft-water localities.
The vital role of magnesium for optimal cardiac function has
recently been reviewed [5, 11]. Similarly, the correlation
between human health and drinking water hardness has been the
subject of a comprehensive report issued by the National Research
Council of Canada [15], in which it was concluded that the intake
of dietary magnesium is sub-optimal in the modern-day world, and
that waterborne magnesium can make a sizeable contribution to the
total daily intake of magnesium in some hard-water regions. The
purpose of this presentation is to attempt to quantify the effect
of waterborne magnesium on human mortality/morbidity, based on
observations reported in several regions of the modern-day
world.
Muss [17] used the data of Schroeder [20] to conduct a
state-by-state intercomparison throughout the continental United
States, and thereby derived the following equation for the linear
interrelation between total cardiovascular (CV) mortality and the
total hardness (TH) of drinking water:
CV deaths / 100,000 = 905.5 - (0.916 X TH).
On this basis, Muss [17] concluded that a TH of 100 would
reduce CV mortality by 10.1 % among white males, age 45-64
years.
This interrelation can be interpreted in terms of waterborne
magnesium, because Schroeder [20] reported the average chemical
composition of drinking water in 163 metropolitan centers
throughout the continental USA. From this, it can be calculated
that water having a TH of 100 contains 8.3 mg/l of magnesium.
And, bearing in mind that Muss [17] had associated this with a
10.1% decrease in CV mortality, it can be further calculated that
a 10% reduction in CV mortality would be conferred by a
waterborne magnesium concentration of 8.2 mg/l.
Note: It is known that waterborne magnesium can
account for a variable proportion of the TH in different
geochemical zones [16]; but nevertheless, in this specific
instance, an 'average' value was sought for the purpose of
interpreting the overall epidemiological trend in the USA.
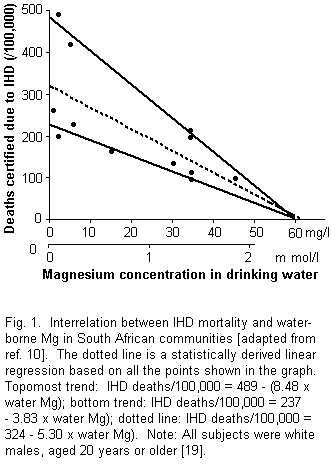
In South Africa, Leary et al. [10] have recently assessed
mortality from ischemic heart disease (IHD) as a direct function
of waterborne magnesium concentrations. As illustrated in figure
1, there appear to be two distinct linear trends, and no ready
explanation can be offered for this disparity. Linear regression
equations were calculated for each trend, and also for the
aggregate of all the points shown in figure 1. On this basis, it
can be calculated that a 10% reduction in IHD mortality would be
conferred by, respectively, a waterborne magnesium concentration
of 5.8, 6.2, and 6.1 mg/l.
Note: It has been suggested [19] that exponential
curves would be a more realistic manner of presenting the data
derived from the US and South African surveys. The point is well
taken. However, curvilinear plots do not readily lend themselves
to a quantitative assessment of the respective trends. (An
exponential approach is illustrated in figure 2, although the
data contained therein will be discussed later in this
presentation.)
When the linear-regression approach is used, it can be seen
that there is a suprising degree of agreement between the US and
South African data, i.e., a 10% reduction in CV or IHD mortality
can be expected with a waterborne magnesium increment of
approximately 8 or 6 mg/l, respectively. Thus, there is an
indication that waterborne magnesium may be more effective in
protecting against IHD mortality than against total CV mortality.
This is compatible with observation made in Canada, where
Anderson [3] intercompared soft water (2 mg/l of Mg) and
hardwater (30 mg/l) localities in Ontario and found that there
were 15-30% more sudden-death IHD fatalities in the soft-water
region, most likely attributable to fatal arrhythmic seizures
induced by an inadequate magnesium intake.
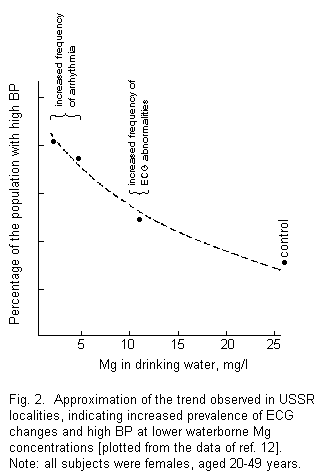
Further light has been shed on this topic by Levin et al. [12]
who studied the influence of drinking water hardness on blood
pressure (BP) and electrocardiographic (ECG) changes in USSR
populations. The strongest correlations were with waterborne
magnesium. Although there was considerable variability in the
clinical data found among various population subgroups, it is
possible to present a graphic illustration of the overall trend
(fig. 2). Note that there was a 3-fold increased prevalence of
high arterial BP at the lowest waterborne magnesium level (2.4
mg/1) in comparison with the 'control' locality (26.2 mg/1).
Also, at progressively lower levels of waterborne magnesium,
there was an increasing frequency of ECG abnormalities until at
very low waterborne magnesium levels - more sinus arrhythmia was
also observed among the population. Thus, the data in figure 2
suggest that moderate increments of waterborne magnesium can have
a noticeable effect on BP and ECG patterns among long-term
residents, and this magnesium-related trend is supported by other
recent studies. For example, there is now experimental evidence
[1] demonstrating that increasing the severity of magnesium
deficiency produces graded elevations of arterial BP. Also,
clinical supplementation of magnesium (360 mg/day, equivalent to
the RDA requirement) reduced both the systolic and diastolic BP
by an average of 13 mm Hg in hypertensive patients during a
6-month period [4]. Concerning ECG patterns, it has been reported
[9] that a bolus oral supplement of 600 mg of magnesium per day
for 4 days prevented postsurgical ECG abnormalities; in the same
study, it was suggested that ECG patterns might be a means of
providing an accurate index of the intracellular myocardial
magnesium status in humans. In this connection, recent work in
China [21] has shown that the early ECG changes in mild magnesium
deficiency are limited to T wave abnormalities, and it was stated
that: 'When neuromuscular irritability exists ... the ECG may
serve as an important clue to pointing out the possibility of
magnesium deficiency.'
Table I. Use of magnesium-rich mineral waters for
therapeutic purposes
----------------------------------------------------------------
Mg dosage,
mg/day Duration Result Reference
----------------------------------------------------------------
90 15 days abated neuromuscular hyperexcitability 6
67-134 3 months improved condition of asthmatics 7
----------------------------------------------------------------
Here, it is appropriate to point out that magnesium-rich
mineral waters have recently been used for therapeutic purposes
(table I), and that one of the findings involved
magnesium-mediated abatement of neuromuscular hyperexcitability.
In table I, it can also be noted that the magnesium dosages were
in the neighborhood of 100 mg/day, and that clinical improvement
was seen within the relatively short timespan of 15 days to 3
months.
All of the aforementioned observations present a consistent
pattern, illustrating the importance of magnesium in protecting
against cardiovascular trauma and other metabolic
aberrations.
In Canada, there has been emphasis on selective depletion of
myocardial magnesium which averaged 6 % lower in subjects
residing in soft-water areas than in individuals residing in
hard-water areas [2]. Such a depletion, even if not fatal,
represents a considerable proportion of the 12-27% magnesium loss
found in non-necrosed myocardial tissue of ischemic and/or
sudden-death cardiac fatalities [5, 16], and is felt to be a
predisposing factor in 'sensitizing' the heart and making it more
vulnerable to stress-induced fatal seizures [3, 14, 18]. An
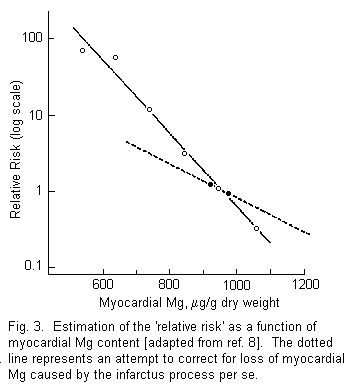
approximation of the enhanced risk has been calculated as a
function of the myocardial magnesium content at autopsy [81, and
this is shown in figure 3. Note that, when the myocardial
magnesium decreases from 1,060 to 550 µg/g, the apparent
relative risk (solid line) increases by a factor of > 100
fold. In figure 3, the dotted line represents an attempt to
correct for loss of myocardial magnesium caused by the
ischemic/necrotic process per se; on this basis, a myocardial
magnesium decrease from 1,220 to 680 µg/g enhances the risk
>10-fold.
In the softest water regions of Ontario, Canada, the average
6% shortfall in myocardial magnesium content occurs in both
cardiac and noncardiac subjects [2]. Furthermore, it has been
estimated that the hardest Ontario waters provide 53 mg more
magnesium per day than do the extremely soft waters [3, 16].
Thus, a 53-mg magnesium supplement per day seems to make a 6%
difference in the magnesium status of the heart; and, bearing in
mind that cardiac fatalities have been associated with an average
18% shortfall of myocardial magnesium [5, 16], then prevention of
myocardial magnesium loss might be expected by providing 18/6 X
53 = 159 mg of supplementary magnesium per day. This is very
close to the daily supplement dosages previously advocated [15],
although the question arises 'What would this mean in terms of
waterborne magnesium?'
An assessment of dietary magnesium intake in 4 diverse regions
of the continental USA has indicated [14] that drinking water
having a TH of 100 would contribute 17 mg of magnesium per day.
At the outset of this presentation, we have already seen that
such waters tend to contain 8.3 mg/l of magnesium. Therefore, in
this context, the intake of water (in all forms, e.g., coffee,
tea, soups, reconstituted beverages etc.) is 17/8.3 = 2 liters
per day. From this, it follows that the aforementioned 159 mg/day
magnesium supplement would require a communal water supply
containing 159/2 = 80 mg/l of magnesium.
Note.- Such water suppliers are uncommon, and this
is why alternate modes of supplementation have also been
discussed [16].
In the previously discussed epidemiological data from the USA
and South Africa, a 10% decrease in cardiac-related mortality was
conferred by a waterborne magnesium increment of 8 or 6 mg/l,
respectively. With an aggregate water intake of 2 liters per day,
this is equivalent to a waterborne magnesium contribution of 16
or 12 mg per day. A similar calculation can be applied to other
water-related observations discussed in this presentation.
Thus, the fact that the waterborne magnesium factor has been
observed in the USA, South Africa, the USSR, and Canada, is
indicative of a global phenomenon which reflects the inadequate
metabolic magnesium status in several regions of the modern-day
world. As previously discussed [15, 16], factors that contribute
to an impoverished magnesium status include an over-dependency on
refined dietary staples, alcohol abuse, chronic digitalis usage,
and long-term diuretic therapy.
One further comment can be made about waterborne magnesium. It
had been suggested [14] that waterborne magnesium may be
approximately one third better absorbed than dietary magnesium,
and recent research in Holland indicates that this may indeed be
the case [13]. If this finding receives extensive corroboration,
this would mean an enhanced metabolic effectiveness of waterborne
magnesium, i.e., greater than an equivalent dosage of dietary
magnesium. However, this aspect must await clarification by
future research.
L'évaluation quantitative du rôle du
magnésium dans l'interrelation entre la
mortalité/la morbidité humaine et la dureté
de 1'eau
Nous avons tenté d'évaluer quantitativement
1'effet du magnésium apporté par 1'eau sur la
mortalité, et la morbidité humaine sur la base
d'observations épidémiologiques et cliniques
rapportées dans plusieurs régions du monde actuel.
Il est apparu une caractéri'stique constante, indiquant un
phénomène mondial qui illustre l'importance du
magnésium apporté par 1'eau dans la protection
contre les affections cardiovasculaires. Ces constatations
attestent l'état métabolique inadéquat chez
l'homme moderne, spécialement dans des localités
avec une eau très douce.
References
1 Altura, B.M.: Magnesium deficiency and hypertension. Nutr.
Rev. 42: 235-236 (1984).
2 Anderson, T.W.; Neri, L.C.; Schreiber, G.; Talbot, P.;
Zdrejewski, A.: Ischemic heart disease, water hardness, and
myocardial magnesium. Can. med. Ass. J. 113: 199-203 (1975).
3 Anderson, T.W.: Water hardness, magnesium, and ischemic
heart disease. Nova Scotia Med. Bull. April: 58-61 (1977).
4 Dyckner, T.; Wester, P.O.: Effect of magnesium on blood
pressure. Br. Med. J. 286: 1847-1849 (1983).
5 Ebel, H.; Gunther, T.: Role of magnesium in cardiac disease.
J. Clin. Chem. Clin. Biochem. 21: 249-265 (1983).
6 Gueux, E.; Poenaru, S.: Duchêne-Marullus, P.:
Electromyographic changes associated with high level of magnesium
in drinking-water. Magnesium-Bull. 2: 154-156 (1982).
7 Haddad, Z.E.: Les effets d'une eau de table riche en
magnésium sur l'asthme bronchial. Allergie Immunol. 14:
11-16 (1982); pers. commun. May 18/84; see also B. Ninard: Med.
Nutr. 13: 53 (1977).
8 Hewitt, D.; Neri, L.C.: Development of the 'water story'-
Some recent Canadian studies. J. Envir. Pathol. Toxicol. 4: 51-63
(1980); pers. commun. June 27/84.
9 Krasner, B.S.; Girdwood, R.; Smith, H.: The effect of
slow-releasing oral magnesium chloride on the Q-T interval of the
electrocardiogram during open-heart surgery. Can. Anaesth. Sec.
J. 28: 329-333 (1981).
10 Leary, W.P.; Reyes, A.J.; Lockett, C.J.; Arbuckle,
D.D.;Vanderbyl, K: Magnesium and deaths ascribed to ischemic
heart disease in South Africa. S. Afr. Med. J. 64: 775-776
(1983).
11 Lehr, D.: Magnesium and cardiac necrosis. Magnesium-Bull.
la: 178-191 (1981).
12 Levin, A.I.; Novikov, Y.V.; Plitman, S.I.; Noarov. Y.A.;
Lastochkima, K.O.: Effect of water of varying degrees of hardness
on the cardiovascular system. Gig. Sanit. 10: 16-19 (1981).
13 Lowik, M.R.H.; Groot, E.H.; Binnerts, W.T.: Magnesium and
public health - The impact of drinking-water. Annu. Symp. Proc.
Univ. Missouri.. Trace substances in environmental health. 16:
189-195 (1982).
14 Marier, J.R.; Cardioprotective contribution of hard waters
to magnesium intake. Revue Can. Biol. 37: 115-125 (1978).
15 Marier, J.R.; Neri, L.C.; Anderson, T.W.: Water hardness,
human health, and the importance of magnesium. National Research
Council of Canada, Report No. 17581 (Ottawa 1979).
16 Marier, J.R.: Quantitative factors regarding magnesium
status in the modem-day world. Magnesium 1: 3-15 (1982).
17 Muss, D.L.: Relationship between water quality and deaths
from cardiovascular disease. J. Am. Water Works Ass. 54:
1371-1378 (1962).
18 Neri, L.C.; Marier, J.R.: Epidemiology of sudden death
minerals and the water story; in Nutrition and heart disease, pp.
81-96 (SP Medical & Scientific Books, Jamaica, N.Y.
1982).
19 Reyes, A.J.: pers. commun. Aug. 23/84; Holanda 1724,
Montevideo.
20 Schroeder, H.A.: Relation between mortality from
cardiovascular disease and treated water supplies. J. Am. med.
Ass. 172: 98/1902 - 104/1908 (1960).
21 Wan-chun, C; Xin-xiang, F.; Shen-jiu, P.; Shaozhen, Q.: ECG
changes in early stage of magnesium deficiency. Am. Heart J. 104:
1115-1116 (1982).
This page was first uploaded to The Magnesium Web Site on June
12, 1996
http://www.mgwater.com/



