Magnesium Trace Elem 1990;9:143-151
Effect of Dietary Magnesium Supplementation in the Prevention
of Coronary Heart Disease and Sudden Cardiac Death
R.B. Singh
Medical Hospital and Research Centre, Moradabad, India
Key Words.
Sudden cardiac death - Coronary heart disease
Abstract: Magnesium may be important in the
pathogenesis of coronary heart disease and sudden death. To study
the role of magnesium, 400 high risk individuals were asked to
volunteer either for a magnesium-rich diet (group A, 206) or for
our usual diet (group B, 194) for 10 years in a randomized
fashion. The age groups were between 25 and 63 years and the
majority (374) of them were males. At entry to the study, age,
sex, incidence of hypertension, diabetes, hypercholesterolemia,
smoking, coronary disease and diuretic therapy were comparable.
Dietary magnesium intake in group A (1, 142 ± 233 mg/day)
was higher than in group B (418 ± 105 mg/day). Total
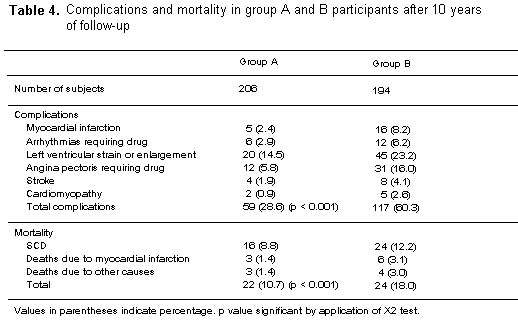
complications in group A (59; 28.6%) were significantly (p <
0.01) less compared to group B (117; 60.3 %). Sudden deaths were
one and a half times more common in group B than in group A.
Total mortality in group A (22; 10.7%) was significantly (p <
0.01) less than in group B (34; 18.0%). A greater number of
complications and increased mortality in group B subjects was
consistent with a higher incidence of hypokalemia, hypomagnesemia
and coronary risk factors in group B patients. Mean serum
magnesium levels in group B participants were significantly (p
< 0.01) lowered compared to the mean magnesium level in group
A participants who were administered the magnesium-rich diet. It
is possible that increased intake of dietary magnesium in
association with the general effects of a nutritious diet can
offer protection against cardiovascular deaths among high-risk
individuals predisposed to coronary heart disease.
Introduction An increased incidence of sudden
cardiac death (SCD) has been observed in soft water areas with
lowered water content of magnesium [1a, 2, 3, 20, 22, 23]. A
lowered myocardial magnesium content has also been demonstrated
in victims dying of SCD and in road accidents in these areas
compared to other areas [12, 22, 23]. The magnesium content of
the infarcted portion of the myocardium was found to be lowered
compared to noninfarcted myocardium [3]. Clinical and
experimental studies emphasize that hypomagnesemia may be
associated with arrhythmias and replacement of magnesium ions has
been suggested [2, 3, 7, 13, 26, 27] and proposed [24, 28] to be
useful in the prevention of sudden deaths due to cardiac
arrhythmias. Diuretic-induced loss of cations can predispose to
sudden deaths among patients with hypertension and coronary
disease, particularly in the setting of acute myocardial
infarction [7, 13].
Epidemiologic studies [14, 181 showed a significant positive
correlation between incidence of ischemic heart disease (IHD) and
the calcium/magnesium ratio of food and water ingested. A
positive correlation was also noted between dietary
sodium/magnesium ratio and incidence of hypertensive heart
disease. A magnesium-deficient diet has been reported to cause a
rise in blood pressures in Wistar rats [lb]. Magnesium deficiency
can influence electrolyte transport across the cell membrane and
enhance coronary artery tone [2, 28]. It may also predispose to
increased adrenergic activity, enhanced vascular reactivity,
spasm, platelet dysfunction and thrombosis [2, 3, 6). Magnesium
administration in acute myocardial infarction can reduce
arrhythmias and mortality [19].
In view of these observations, the purpose of this study was
to examine the effect of dietary magnesium in the prevention of
IHD and SCD among high-risk free living individuals.
Material and Methods
The study dietitian recruited urbanized adults with major or
minor risk factors, with or without cardiovascular disease, by
advertisements in the local clubs and newspapers. Respondents
having cancer, chronic renal failure, chronic diarrhea and
dysentery or who felt unable to participate were excluded from
this study. Clinical, electrocardiographic, radiologic and
laboratory data were obtained in all the participants during 2
weeks of surveillance before admission to the study. Exercise
electrocardiograms were done to confirm the presence or absence
of IHD in all the participants. Blood pressures were measured
after 5 min of rest lying comfortably in a supine position, by a
mercury sphygmomanometer by the same person. Korotkoff sounds,
phase V, were recorded for diastolic blood pressure. Hypertension
was diagnosed in the presence of blood pressures above 150/95 mm
Hg, diabetes by a positive glucose tolerance test, smoking by
consumption of more than 10 cigarettes/day, obesity by 10 % more
weight than normal for that age and sex. Hypercholesterolemia was
diagnosed in the presence of fasting serum cholesterol of more
than 250 mg/dl. Presence of these major and/or minor risk factors
of IHD was considered a high risk for the study population. The
diagnosis of IHD, arrhythmias, ischemia, prolonged Q-T interval,
left ventricular strain or elements and physical inactivity was
based on criteria laid down by the WHO [30].
Laboratory data included blood urea, sugar, total cholesterol,
low- and high-density lipoprotein cholesterol, total blood
leukocytes, hemoglobin, serum sodium potassium [29], magnesium
[8], calcium [17] and albumin. The criteria of SCD was death
occurring within 1 h either due to IHD or without any apparent
cause. The study dietitian divided all the participants into two
groups alternately in a randomized fashion after informed consent
and the physician responsible was blinded to dietary regimens.
Group A included persons on a magnesium-rich dietary protocol and
group B included persons on our usual diet. Participants who
discontinued the trial during follow-up were excluded. Only those
participants who completed a minimum of 10 years have been
included in the analysis of the data.
The aim during the study period was to achieve a stable body
weight on the lower side of normal weight for that age, sex and
height. The diets for the obese and hyperlipidemic persons were
lower in total fat content and had the same ratio of
polyunsaturated fatty acids to saturated fatty acids that are
recommended for group A subjects. Consumption of energy by
different individuals ranged from 1,200 kcal to 2,500 kcal, and
nutrients were adjusted accordingly in both of the groups. The
distribution of various nutrients in the diet taken by the two
groups (obtained by food composition tables [9]) is shown in
table 1. In the magnesium-rich diet, fruits, green vegetables,
cereals and nuts were given to group A participants.

Dietary advice was reinforced vigorously and regularly at 1-4
weekly visits to all participants in particular to those with
risk factors for coronary disease, e.g., diabetes, hypertension,
hypercholesterolemia, myocardial infarction and angina. All of
the participants completed dietary diaries beginning at week 2,
week 4, week 6, week 12 and then every 12 weeks (biannually in
asymptomatic subjects without risk factors) to assess dietary
compliance. Each participant was asked regularly to follow,
closely, the dietary advice and fill out a questionnaire
regarding dietary intakes at separate counseling sessions by the
dietitian and the physician, respectively. The dietitian also
made home visits to educate housewives regarding the maintenance
of dietary compliance. Apart from dietary diaries, evidence of
dietary compliance of the experimental diets, in both groups, was
obtained by measuring the serum magnesium in some randomly
selected patients at the beginning of weeks 0. 4 and later once
per year. We noted a sustained rise in the amount of serum
magnesium confirming dietary compliance with the experimental
diet.
Follow-up in all symptomatic participants and those with major
risk factors for coronary artery disease was made at weeks 1-4
for the entire period and in others at weeks 6-12 for 1 year and
later on a biannual basis for 10 years. In those healthy
participants who were reluctant to come, details were obtained by
telephone, letter and personal visits, whichever was
applicable.
Results
Of the 442 respondents, 12 were excluded and 30 cases left the
trial before it was completed. The dietary specifications,
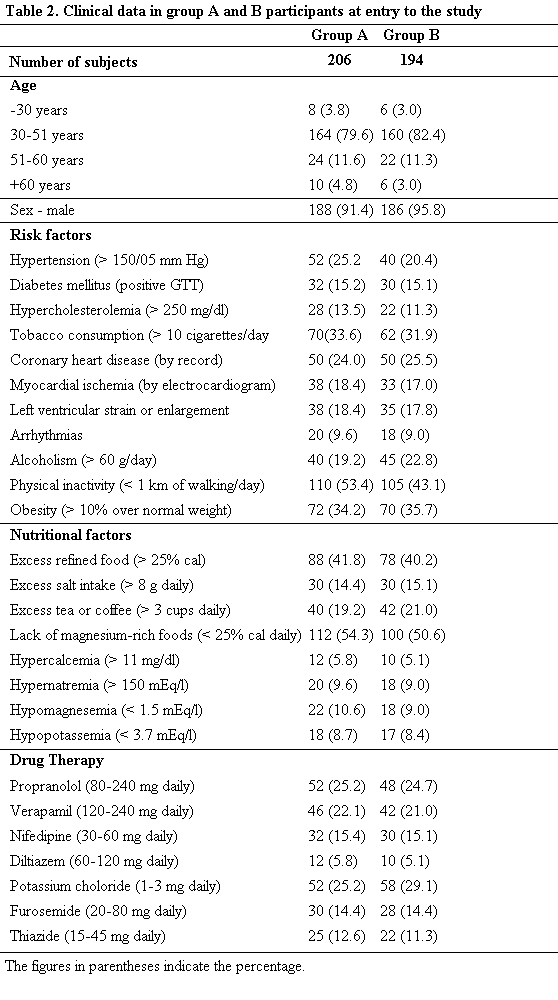
clinical and laboratory data in the remaining 206 group A and 194
group B patients exhibiting alteration in risk factors are shown
in tables 1-3. At entry to the study, there was no significant
difference in the proportion of patients in age groups, sex, risk
factors, coexisting complications of atheromatous diseases,
dietary factors, miscellaneous factors and drugs between the two
groups. The incidence of patients with hypomagnesemia and
hypokalemia was similar as were other laboratory data in all the
patients. A similar rehabilitation program for risk factor
modification was followed in both of the groups. The differences
in the dietary intakes are shown in table 1. Intervention diet
(group A) included increased intake of fruits, vegetables,
cereals and nuts which amounted to around 2.5 times more intake
of magnesium and potassium in this group compared to control
group B. Smoking, alcoholism and drug therapy remained comparable
in both the groups. Study of the pattern of risk factor
modification showed that smoking was reduced or stopped in 24
patients in group A and 28 patients in group B. Obesity was
corrected for 23 patients in group A and 17 in group B.
Hypercholesterolemia was corrected for 19 patients in group A and
14 in group B. Alcohol intake was occasional in 12 patients in
group A and 15 in group B. Hypokalemia [21] and hypomagnesemia
[22] became more common in group B, whereas there was no such
deficit in group A at end of the study.
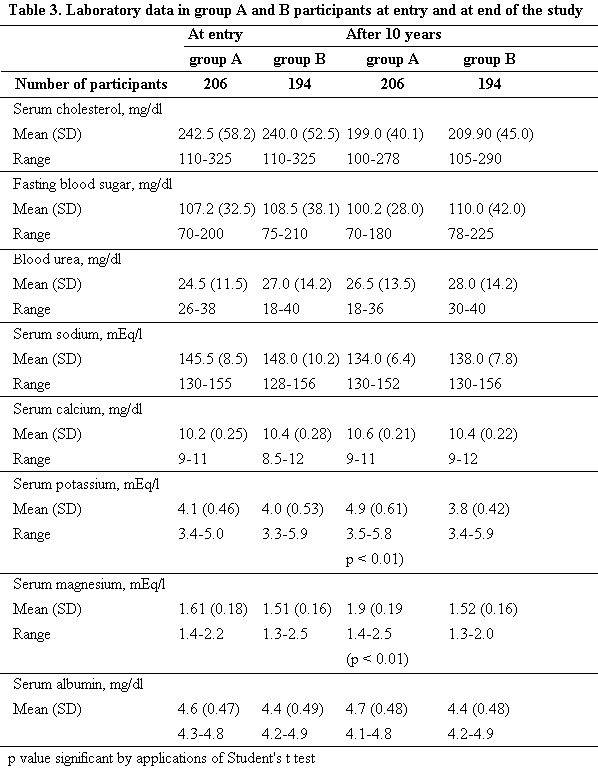
Initial mean serum cholesterols were in the high to normal
range without a significant difference between the two groups
(table 3). After 10 years of magnesium-rich dietary therapy in
group A, and our usual diet in group B, there was a significant
fall in serum cholesterol in both groups compared to basal levels
but without a significant difference between the two groups.
There was no significant difference in the incidence of
hypokalemia, hypomagnesemia, IHD, angina and arrhythmias between
the two groups, initially. However, after 10 years, the incidence
of predisposing factors such as hypokalemia, hypomagnesemia and
total complications such as IHD, angina and arrhythmias were
significantly higher in group B compared to the intervention
group (tables 2-4).
There was a rise in serum magnesium and potassium in
participants with deficiency of these cations in group A compared
to no such rise in group B participants with a similar deficit.
The majority of these patients with mineral deficits,
particularly hypokalemia and hypomagnesemia, were hypertensives
receiving diuretics. The mean serum magnesium and potassium
levels after the study in total number of
mineral-rich-diet-supplemented group A patients were also
significantly higher compared to the mean levels of these cations
in group B patients given our usual diet (table 3).
Sudden Cardiac Death
The incidence of sudden death and deaths due to IHD in group A
(19; 10.2 %) was significantly (p < 0.02) less compared to
such deaths (30; 1 5.2 %) in group B (table 4). This complication
occurred mostly in males between 51 and 60 years of age. The
majority of them had IHD or risk factors for coronary disease. A
few victims in group B had frank hypomagnesemia (2 cases) and
hypokalemia (3 cases) in contrast to the absence of such changes
in the intervention group.
Discussion
During the last five decades, there has been a sharp increase
in the prevalence of cardiovascular diseases and sudden IHD
deaths following increased intake of saturated fat, refined and
preserved food and diminished intake of fruits, vegetables and
cereals [1a, 22]. Underlying this syndrome is the tremendous
increase in the incidence of atherosclerosis, hypertension and
acute myocardial infarction in young age groups. One experimental
study [26] showed that a diet rich in saturated fat, cholesterol,
vitamin D, sodium, phosphate, animal proteins and low in
magnesium, potassium and polyunsaturated fat given to rats was
associated with an increased number of myocardial infarctions,
coronary atherosclerosis and hypertension, factors which are now
considered to predispose to SCD [la, 10, 24, 25]. Animals on such
an experimental diet retained more body sodium, 12% more
myocardial calcium and a drop of 19% magnesium and 33 % potassium
in the myocardium and 20% of both cations in the serum [26). In a
more recent study for dietary prevention of coronary heart
disease, there was a significant reduction in the incidence of
sudden death in the intervention group compared to control
subjects [10].
Recently, major attention has been paid to antiarrhythmic
measures and myocardial factors which produce arrhythmias
contributing to SCD [5]. Indeed, more attention should be given
to the total spectrum of sudden death cases which involves
occurrence of arrhythmias in the setting of IHD [15, 21]. It is
possible that changes in life-style and dietary habits which
reduce blood cholesterol and IHD mortality might diminish SCD
[10, 251. In view of the above studies, showing the relation of
nutritional factors and IHD with sudden death, the observations
of the present study seem to be logical. It is possible that
correction of magnesium and potassium deficiency and increased
body status of these cations in association with blood
cholesterol reduction offered protection to group A participants
against IHD and SCD. Similarly, a low cation status in the
presence of hypomagnesemia and hypopotassemia, particularly in
the setting of IHD, left ventricular dysfunction and arrhythmia
could have precipitated a greater incidence of total
complications, sudden deaths and total mortality in group B.
Increased intake of dietary magnesium and pharmacological
magnesium administration have been found to be protective against
atheromatous diseases [1a, 22, 23] and mortality in patients with
acute myocardial infarction [19]. It was not possible in our
study, however, to separate the effect of hypocholesterolemia and
hypokalemia in group A patients from that of hypomagnesemia.
Reduction in cholesterol showed no influence upon mortality from
SCD [15, 21 ] but the reduction in blood cholesterol in group A
on total mortality seems to be important [16].
In the majority of SCD, the underlying mechanism is
ventricular fibrillation which involves electrophysiologic
changes due to metabolic and biochemical alterations, occurring
across the myocardial cell membrane. These factors in turn may be
under the influence of nutrients in the serum and the cells [1a,
2]. One experimental study [4] showed that coronary arterial
reperfusion may be associated with an increase in myocardial
tissue water and potassium, loss of magnesium and minimal changes
in calcium and sodium ions. A clinical study [11] showed cellular
deficiency of magnesium, potassium and zinc during exercise and
stress in type A personality subjects. These studies and
observations of the present work indicate that magnesium in
association with other dietary factors may have a role not only
in the pathogenesis of IHD and SCD but also in their prevention,
particularly in patients with major risk factors for IHD.
Acknowledgements
I am grateful to Vipin for secretarial help and to Sushav,
Reema and Kartick for support.
References
1a Altura, B.M.: Ischemic heart disease and magnesium.
Magnesium 7: 57-67 (1988).
1b Altura, B.M.; Altura, B.T.; Gebrewold, A.; Ising, H.;
Gunther, T.: Magnesium deficiency and hypertension, correlation
between magnesium deficient diet and microcirculatory changes in
situ. Science 223: 1315-1317 (1984).
2 Altura, B.M.; Altura, B.T.: Magnesium electrolyte transport
and coronary vascular tone. Drugs 28: 120-142 (1984).
3 Altura, B.M.; Altura, B.T.: New perspective on the role of
magnesium in the pathophysiology of cardiovascular system.
Clinical aspects. Magnesium 4: 226-244 (1985).
4 Basuk, W.L; Reimer, K-L; Jennings, R.B.: Effect of
repetitive episodes of ischaemia on cell volume, electrolytes and
ultrastructure. J. Am- Coll. Cardiol. 8: 33A-41A (1986).
5 Bigger, J.T.; Fleiss, J.L; Kleiger, R.L; Miller, J.R.;
Rolnitzsky, LM.; the multicentre postinfarction research group:
T'he relationship among ventricular arrhythmias, left ventricular
dysfunction and mortality in two years after myocardial
infarction. Circulation 69: 250-255 (1981).
6 Chadda, K-D.; Essman, E.J.; Schultg, N.: Alpha adrenergic
receptors and induced hypomagnesemia. Magnesium 2: 125-131
(1983).
7 Dyckner, T.; Wester, P.O.: Clinical significance of
diuretic-induced magnesium loss. Pract. Cardiol. 10: 124-133
(1984).
8 Gindler, E.M.; King, J.D.: Determination of calcium in
plasma. Am. J. clin. Path. 58: 376-386 (1972).
9 Gopalan, C.; Rama Sastri, B.V.; Balasubramanium, S.C.:
Nutrition value of Indian foods (National Institute of Nutrition.
Publication, Hyderabad 1976).
10 Hajermann, I.; Holm, I.; Gyre, K.V.; Leren, R.: Effect of
diet and smoking intervention on the incidence of coronary heart
disease. Report from the Oslo study group of a randomized trial
in healthy men. Lancet i.: 1303-1310 (1981).
11 Henrotte, J.G.; Ploin, P.F.; Levy, L.D.; et al.: Blood
erythrocyte and urinary magnesium, zinc, calcium, free fatty
acids and catecholamines in type A and B subjects. J. Am. Coll.
Nutr. 4: 165- 172 (1985).
12 Johnson, C.J.; Peterson, D.R.; Smith, E.K.: Myocardial
tissue concentrations of magnesium and potassium in men dying
suddenly from ischemic heart disease. Am. J. clin. Nutr. 32:
960-967 (1971).
13 Kaplan, N.M.: Our appropriate concern about hypokalemia.
Am. J. Med. 77: 1-5 (1984).
14 Karppanen, N.: Epidemiological studies on the relationship
between magnesium intake and cardiovascular disease. Artery 9:
190-199 (1981).
15 Kannel, W.B.; Schatskin, A.: Sudden death: lesions from
subsets in population studies. J. Am. Coll. Cardiol. 5: suppl. 6,
p. 141B (1985).
16 Kesteloot, H.: Nutrition and cardiovascular disease. Acta
cardiol. 42: 73-77 (1987).
17 Khayam-Bashi, H.; Liu, TJ.; Walter, B.: Determination of
serum magnesium by calorimetric method. Clin. Chem. 23: 289-300
(1977).
18 Marier, J.L: Role of environmental magnesium in
cardiovascular disease; in Wanto, Nutrition and heart disease,
pp. 31-59 (Medical and Scientific Books, New York 1982).
19 Rasmussen, H.S.; McNair, P.K.; Morregord, P.; et al:
Intravenous magnesium in acute myocardial infarction. Lancet i:
234-236 (1986).
20 Schroeder, H.A.: Municipal drinking water and
cardiovascular death rates. JAMA 95: 125-135 (1966).
21 Schatskin, A.; Cupples, LA.; Heeren, T.; Moreleck, S.;
Mucatcl, M.; Kannel, W.B.: The epidemiology of sudden unexpected
death: risk factor for men and women in the Framingham Heart
Study. Am. Heart J. 107: 1300-1310 (1984).
22 Seelig M.S.; Heggtvcit, H.A.: Magnesium interrelationships
in ischaemic heart disease. Am. J. clin. Nutr. 27: 59-75
(1974).
23 Singh, R.B.; Singh, V.P.; Cameron, E.A.: Magnesium in
atherosclerotic cardiovascular disease and sudden death. Acta
cardiol. 36: 411-429 (1981).
24 Singh, R.B.: Effect of dietary minerals on the incidence of
sudden cardiac death. Trace Elem. Med. 7: 19-24 (1990).
25 Singh, R.B.: Multifactorial risk factor intervention for
sudden cardiac death: the Indian diet heart preliminary study. J.
Adv. Med. 2: 475-485 (1989).
26 Sos, J.: An investigation into the nutritional factors of
experimental cardiopathy. Electrolytes cardiovasc. Dis. 1:
167-180 (1965).
27 Szclenyi, I.: Physiological interrelationship between
magnesium and the heart; in Durlach, International Symposium on
Magnesium, Vittel 197 1, pp. 195-21 1.
28 Turlapaty, P.D.M.V.; Altura, B.M.: Magnesium deficiency
produces spasms of coronary arteries: relationship to etiology of
sudden cardiac death. Science 208: 198-200 (1980).
29 Varley, H.; Gowealock, A.H.; Bell, M.: Sodium, potassium
and chloride by flame photometer. Prac. Clin. Biochem., pp.
850-900 (Heinemann Medical Books, London 1980).
30 World Health Organization: Rehabilitation and comprehensive
secondary prevention after acute myocardial infarction, pp. 5-15
(WHO, Geneva 1983).
R.B. Singh, MD, FICN
Director, Cardiologist and
Professor of Clinical Nutrition (Hon.)
Civil Lines
Moradabad 10 (India)
This page was first uploaded to The Magnesium Web Site on June
19, 1996
http://www.mgwater.com/




